Reconstructive Surgery
Post-Mastectomy Breast Reconstruction
A mastectomy — the surgical removal of one or both breasts as part of breast cancer treatment — is a profound medical and emotional experience. Post-mastectomy breast reconstruction is a reconstructive plastic surgery procedure designed to rebuild the breast mound and restore natural symmetry and body contour. This is not cosmetic surgery in the conventional sense — it is an integral part of the oncological care continuum, carried out in close coordination with the treating oncology team. Reconstruction may be performed on one breast (unilateral) or both (bilateral), and can be completed in a subsequent stage with nipple-areola complex reconstruction.
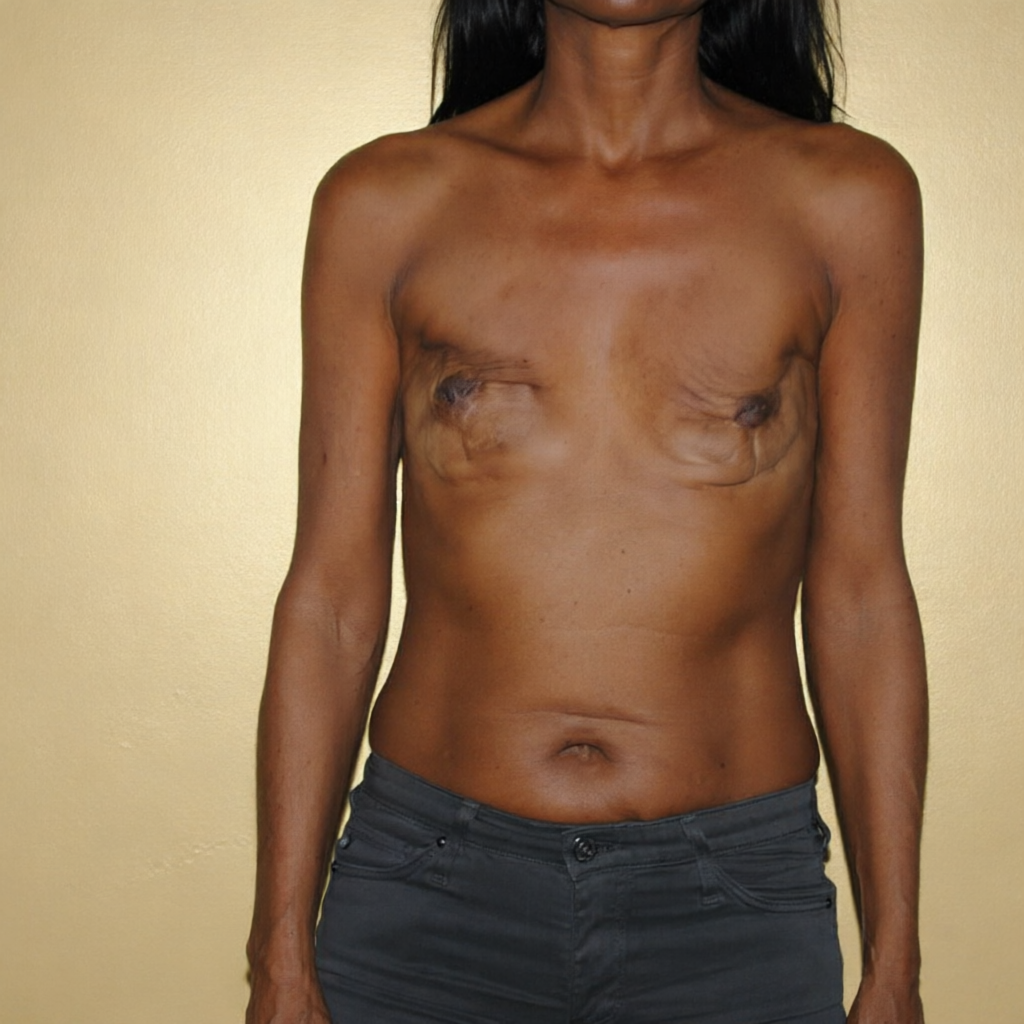
Before
Swipe to compare
Tap to enlarge
What Is Post-Mastectomy Breast Reconstruction?
A mastectomy — the surgical removal of one or both breasts as part of breast cancer treatment — is a profound medical and emotional experience. Post-mastectomy breast reconstruction is a reconstructive plastic surgery procedure designed to rebuild the breast mound and restore natural symmetry and body contour. This is not cosmetic surgery in the conventional sense — it is an integral part of the oncological care continuum, carried out in close coordination with the treating oncology team. Reconstruction may be performed on one breast (unilateral) or both (bilateral), and can be completed in a subsequent stage with nipple-areola complex reconstruction.
Key Benefits
- Improves quality of life and body image in more than 80% of patients
- Multiple techniques: tissue expander, autologous DIEP flap, latissimus dorsi flap
- Immediate or delayed reconstruction depending on oncological pathway
- Multidisciplinary coordination with the treating oncology team
- Optional nipple-areola reconstruction in a third stage
- Partial or full financial coverage possible through insurance
Ideal Candidates
Ideal Candidates
- Any woman who has undergone total or partial mastectomy, whether recently or years ago
- Women in remission or stable during active treatment, in sufficient general health
- Non-smokers or those who have stopped smoking at least 6 weeks before the procedure
- Patients with realistic expectations who understand the multi-stage nature of some reconstruction pathways
- Reconstruction is possible years after mastectomy — there is no upper time limit
Contraindications
- Prior radiotherapy (influences technique selection, not an absolute contraindication)
- Significant obesity (increased complication risk)
- Uncontrolled cardiovascular conditions or diabetes
- Ongoing anticoagulant therapy
Dr. Nahed Fathi Ahmed's Approach and Techniques
Duration: 2 to 5 hours depending on technique
1
Comprehensive pre-operative consultation
Thorough evaluation: medical history review, oncological dossier, clinical examination, imaging, and standardised photographs. Dedicated time for understanding the patient's experience, expectations, and practical constraints.
2
Multidisciplinary coordination
Dr. Fathi liaises directly with the oncologist and breast surgeon to align reconstruction timeline with adjuvant therapies (chemotherapy, radiotherapy, hormone therapy).
3
Tissue expander and implant (two-stage)
A temporary tissue expander placed beneath the pectoralis major muscle to expand the skin envelope. In a second procedure, replaced with a permanent silicone gel implant. Suited to patients with adequate skin quality.
4
Latissimus dorsi flap
A section of skin and muscle from the back tunnelled to the chest to reconstruct the breast mound, usually combined with an implant for volume. Reliable technique, particularly valuable after radiotherapy.
5
DIEP flap (autologous microsurgical reconstruction)
Microsurgical technique using skin and fat from the lower abdomen to reconstruct the breast without any artificial implant. Fully autologous, naturally soft result that ages with the patient.
6
Nipple-areola reconstruction
Optional third stage performed as an outpatient procedure several months after the main reconstruction, using a local flap technique and/or medical tattooing.
Recovery Timeline
Recovery timeline
Day 1–3
Moderate pain, fatigue, swelling. Rest, pain management, personal support.
Day 4–14
Progressive improvement, drain removal. Light activity, no lifting.
Weeks 3–6
Return to daily life. Avoid intense physical exertion, protect scars.
Months 2–3
Partial result visible, scars maturing. Scar massage, silicone gel as prescribed.
Months 6–12
Final result achieved, scars faded. Follow-up visit, nipple reconstruction discussion.
Post-operative care
- Wound dressings and drain care as needed
- Fitted post-surgical bra or compression garment provided
- Follow-up appointments at Day 7, Day 21, Month 3, and Month 6
- Scar massage and silicone gel on prescription
Important restrictions
- No heavy lifting for 4 to 6 weeks
- No intense physical exertion for 6 to 8 weeks
- Sun protection for incision sites mandatory
Recovery and Results
Results timeline
Convalescence varies by technique. Normal daily activity resumed within 4 to 8 weeks. Final aesthetic result visible at 6 to 12 months.
Longevity
For autologous techniques such as the DIEP flap, the reconstructed breast is composed entirely of the patient's own tissue and ages naturally. Complementary adjustments (contralateral symmetrisation, lipomodelling) can be proposed.
What to expect
- Balanced silhouette with discreet scars
- Significant improvement in body image and wellbeing
- Natural autologous result (DIEP flap) or excellent aesthetic with modern implant
- Optional nipple-areola reconstruction in a third stage
See our results
Discover our patients' transformations
Pricing
Estimated price
Fee upon consultation
This price includes
- Comprehensive pre-operative consultation with full workup
- Surgical procedure and hospital stay
- Post-operative compression garment
- Regular follow-up appointments
- Administrative support for insurance reimbursement dossier
Prices shown are estimates and may vary depending on the complexity of your case. A personalized quote will be provided during your consultation.
Frequently Asked Questions
Yes, but radiotherapy alters tissue elasticity and vascularity. In irradiated patients, Dr. Fathi generally favours autologous reconstruction techniques (DIEP or latissimus dorsi flap). Each case is assessed individually.
Absolutely. There is no upper time limit. Dr. Fathi has performed successful reconstructions on patients more than ten years after their mastectomy.
For single-stage implant reconstruction, results visible in 3 to 6 months. For two-stage expander-to-implant, 6 to 12 months. Full autologous DIEP reconstruction with nipple reconstruction may extend to 12 to 24 months.
For autologous techniques like the DIEP flap, the reconstructed breast is composed entirely of the patient's own tissue and has a consistency very similar to a natural breast. Complementary adjustments can optimise symmetry.
No. Reconstruction is planned in collaboration with the oncology team to avoid interfering with adjuvant treatments or surveillance imaging. Modern reconstruction techniques do not impair detection of a potential recurrence.
Coverage depends on the patient's insurance provider and country of origin. Many European private health insurance plans cover reconstructive surgery following cancer treatment. Dr. Fathi's team assists in preparing reimbursement documentation.
Questions about reconstruction-mammaire-post-mastectomie?
Chat directly with our team on WhatsApp for a quick and personalized response.