Breast Surgery
Capsulectomy
When a breast implant is placed, the body responds naturally by forming a thin layer of fibrous connective tissue around the implant: the fibrous capsule. In most patients, this capsule remains soft and imperceptible. In a subset of patients, it thickens, calcifies, and contracts — compressing the implant and distorting the shape and texture of the breast. Capsulectomy is the surgical procedure to remove all or part of this fibrous capsule, followed by a joint decision with the patient regarding the fate of the underlying implant.

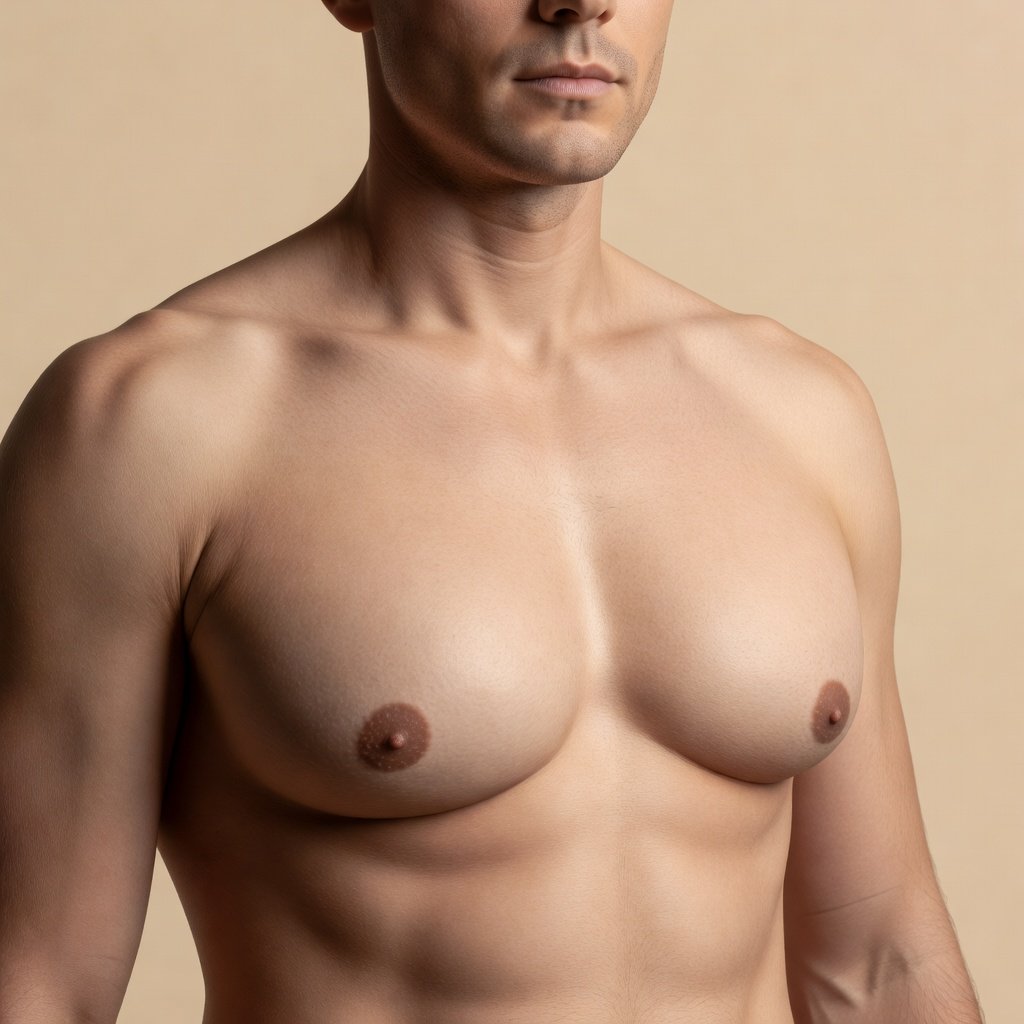
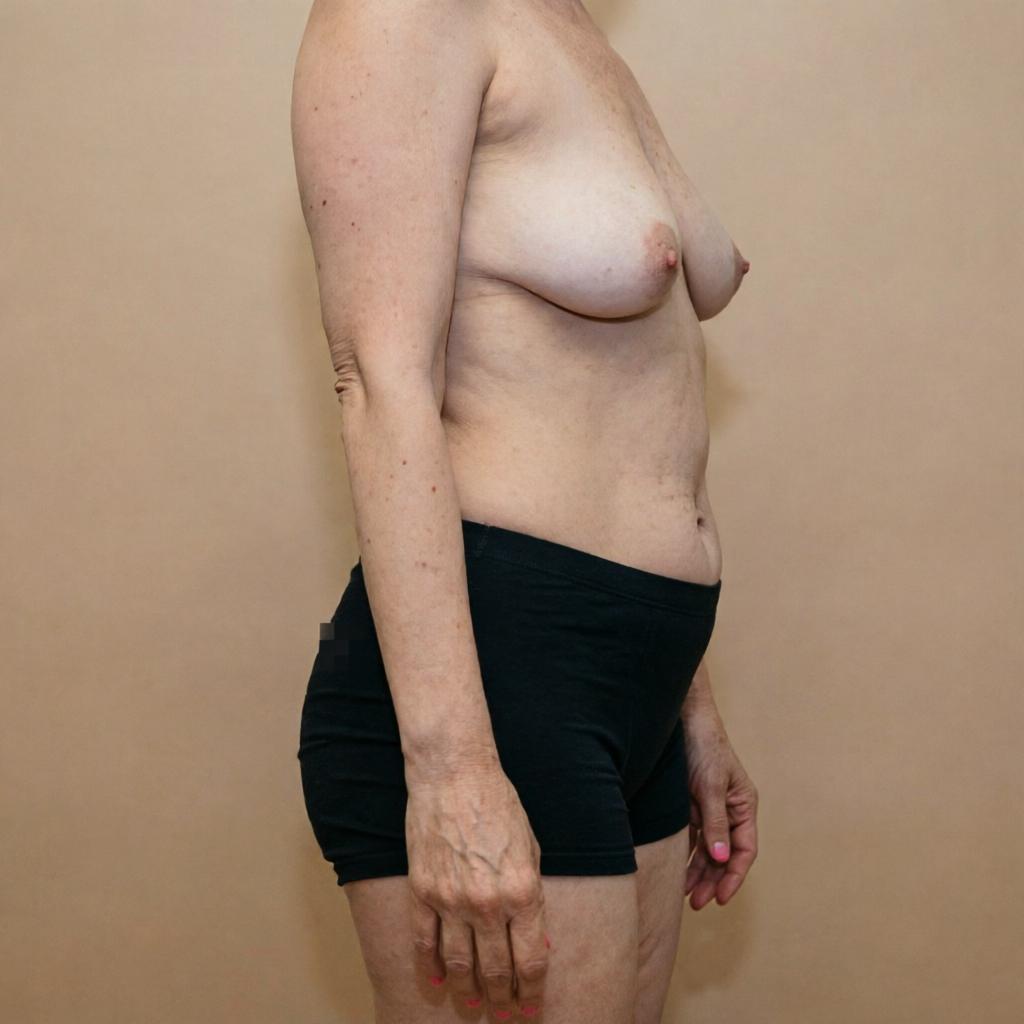
Before
Swipe to compare
Tap to enlarge
What Is Capsulectomy?
When a breast implant is placed, the body responds naturally by forming a thin layer of fibrous connective tissue around the implant: the fibrous capsule. In most patients, this capsule remains soft and imperceptible. In a subset of patients, it thickens, calcifies, and contracts — compressing the implant and distorting the shape and texture of the breast. Capsulectomy is the surgical procedure to remove all or part of this fibrous capsule, followed by a joint decision with the patient regarding the fate of the underlying implant.
Key Benefits
- Resolution of capsular contracture (Baker Grade III–IV)
- Treatment of confirmed or suspected implant rupture
- Options: simple explantation, implant replacement, or simultaneous mastopexy
- Rigorous pre-operative imaging protocol (ultrasound + MRI when indicated)
- En-bloc technique for severe cases preserving capsule containment
- Existing incision sites used — no additional scarring in most cases
Indications and Candidacy
Ideal Candidates
- Capsular contracture Baker Grade III–IV
- Breast implant rupture confirmed or suspected on imaging
- BIA-ALCL diagnosed or suspected
- Chronic pain attributed to the capsule or implant
- Personal choice of explantation
- Implant exchange (replacement with modern implants, volume change)
Contraindications
- Active smoking
- Uncontrolled coagulation disorder
- Active local infection
- Incomplete oncological workup
Dr. Nahed Fathi Ahmed's Surgical Approach
Duration: 1.5 to 3 hours
1
Pre-operative consultation with imaging workup
Breast ultrasound as first-line investigation, supplemented by breast MRI when rupture is suspected or ultrasound is inconclusive. Characterisation of capsule state and implant integrity.
2
General anesthesia
The procedure is performed under general anesthesia.
3
Periareolar or inframammary incision
In most cases, Dr. Fathi uses the existing incision sites from the original implantation — no new scars are added.
4
Capsule dissection and resection
Partial capsulectomy (thickened anterior portion) or total en-bloc capsulectomy (entire capsule intact with implant inside, not opened) depending on Baker grade and indication.
5
Implant removal
Implant extraction according to the chosen technique (partial or en-bloc).
6
Associated procedure per patient choice
Simple explantation, placement of new modern cohesive implants, or mastopexy to correct secondary breast ptosis.
Recovery and Follow-Up
Recovery timeline
Days 1–3
Moderate chest pain, mandatory surgical support bra.
Week 1–2
Swelling and bruising, suture removal at Day 12–14 if non-resorbable.
Week 3–4
Significant improvement in comfort, return to light activities.
Month 1–3
Progressive tissue softening, visible and stable results.
Month 6–12
Scars in maturation phase, final result established.
Post-operative care
- Surgical support bra worn 24 hours/day for 4 weeks
- Protection of existing scar sites
- Avoid activities that engage the pectoral muscles
Important restrictions
- Intense physical exertion (sport, lifting) contraindicated for 6 weeks
- No swimming before full wound healing
Results and Follow-Up
Results timeline
Results visible and stable from months 1–3. Scar maturation over 6 to 12 months.
Longevity
After explantation without replacement, breast tissues restructure progressively over 3 to 6 months. Outcome depends on skin quality and implant wear duration. Mastopexy can be scheduled 3 to 6 months after if residual ptosis is noted.
What to expect
- Resolution of contracture and functional discomfort
- Harmonious aesthetic result according to chosen option
- No new additional scarring in the vast majority of cases
- Progressive improvement over 3 to 6 months
See our results
Discover our patients' transformations
Pricing — Personal Consultation
Estimated price
Fee upon consultation
This price includes
- Pre-operative consultation with imaging workup
- Surgical procedure and hospital stay
- Surgical support bra
- Post-operative follow-up
Prices shown are estimates and may vary depending on the complexity of your case. A personalized quote will be provided during your consultation.
Frequently Asked Questions
Warning signs include progressive firmness of one or both breasts, a change in breast shape (higher, rounder, asymmetric), or pain on palpation. Only a consultation with imaging can confirm the diagnosis.
Yes, in the vast majority of cases. Following total capsulectomy and a healing period, placement of new implants is possible. Dr. Fathi evaluates residual tissue quality at consultation.
BIA-ALCL is a rare lymphoma associated primarily with highly textured surface implants. It typically manifests as a late peri-implant seroma. When diagnosed early, it carries an excellent prognosis and is treated with en-bloc capsulectomy.
In most cases, Dr. Fathi uses the existing scars from the original implantation. No additional incisions are required unless a mastopexy is performed simultaneously.
Breast tissues restructure progressively over 3 to 6 months. The outcome depends on skin quality and how long implants were carried. Mastopexy can be scheduled 3 to 6 months after if residual ptosis is noted.
Breast ultrasound is the first-line investigation. MRI is prescribed when rupture is suspected on ultrasound or when findings are inconclusive. MRI is the reference modality for assessing silicone implant integrity.
Questions about capsulectomie?
Chat directly with our team on WhatsApp for a quick and personalized response.