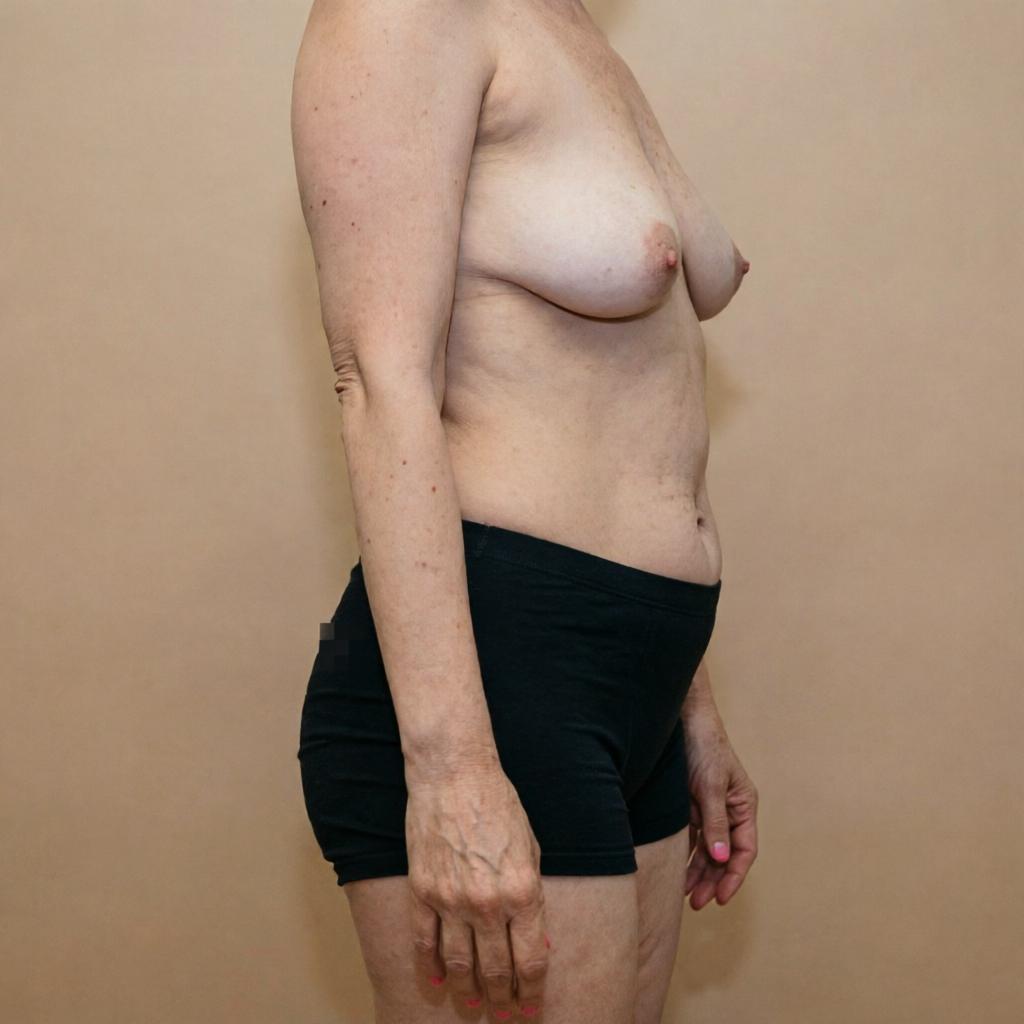
Breast Surgery
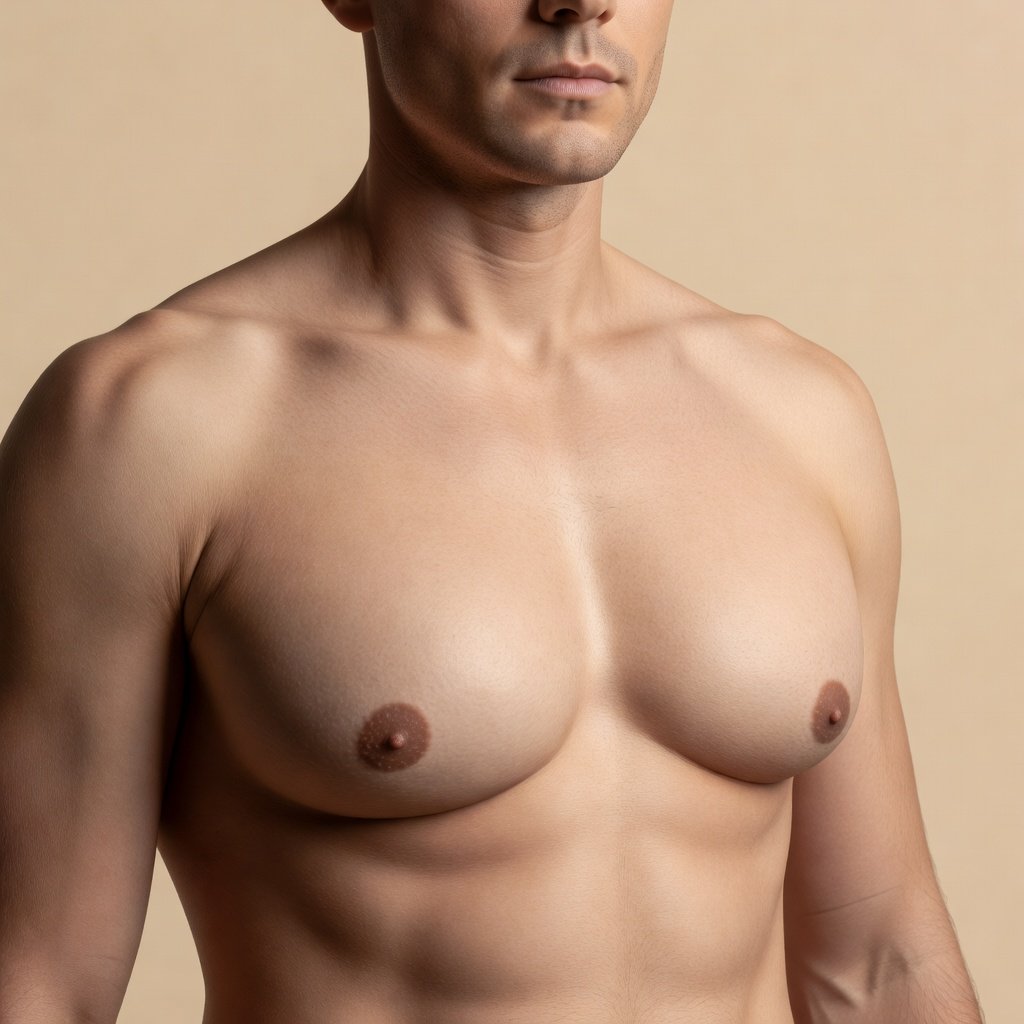
Mixed Gynecomastia
Mixed gynecomastia in men is an abnormal enlargement of breast tissue combining a glandular component and a fatty component, which can only be definitively corrected through surgery combining glandular excision and liposuction. Dr Nahed Fathi Ahmed, plastic surgeon in Agadir, SOMCEP 2024–2025 evaluating member, trained at CHU Avicenne in Rabat, performs this procedure using a precise combined technique that guarantees a flat, natural-looking chest free of any deformity. Gynecomastia affects between 32% and 65% of men at some point in their lives. With over 15 years of experience and 188 procedures performed, Dr Fathi offers personalised care for each case.
Before
Swipe to compare
Tap to enlarge
Overview
Mixed gynecomastia in men is an abnormal enlargement of breast tissue combining a glandular component and a fatty component, which can only be definitively corrected through surgery combining glandular excision and liposuction. Dr Nahed Fathi Ahmed, plastic surgeon in Agadir, SOMCEP 2024–2025 evaluating member, trained at CHU Avicenne in Rabat, performs this procedure using a precise combined technique that guarantees a flat, natural-looking chest free of any deformity. Gynecomastia affects between 32% and 65% of men at some point in their lives. With over 15 years of experience and 188 procedures performed, Dr Fathi offers personalised care for each case.
Ideal Candidates
Ideal Candidates
- Adult male (18 years or older, after hormonal stabilisation)
- Persistent enlargement for at least 6 to 12 months
- Stable weight — not on an intensive diet or experiencing recent weight gain
- Non-smoker or abstained for at least 4 weeks
- Normal preoperative workup (including hormonal panel)
- Realistic expectations
Contraindications
- Adolescents still undergoing hormonal maturation
- Gynecomastia secondary to an untreated medical cause (hypogonadism, hyperthyroidism, testicular tumour)
Procedure
Duration: 1.5 to 2.5 hours
1
Periareolar glandular excision
Fine incision along the lower border of the areola; direct resection of the glandular disc (essential in true gynecomastia)
2
Peripheral Lipomatic Eva6 liposuction
Aspiration of peripheral fatty tissue using mechanical vibrations, preserving vascular and nerve structures, for harmonious chest contouring
3
Symmetry check and closure
Verification of bilateral balance before suturing; any necessary adjustments for a perfectly balanced result
Recovery
Recovery timeline
Days 1–3
Moderate pain, sensation of chest pressure — prescribed analgesics
Week 1
Light activities resumed; no heavy lifting; showering allowed from Day 3
Weeks 2–3
Return to desk work possible; bruising fading
Week 6
Compression vest removed; light sport resumed
Month 3
Stable final result; periareolar scar fading
Months 6–12
Virtually invisible scar; permanent flat, harmonious chest
Post-operative care
- Compression vest worn continuously for 6 weeks, day and night (except for showering)
- Consultations at Day 7, Day 14, Month 1 and Month 3
Important restrictions
- No bodybuilding or contact sport for 3 months
- Light activities (walking, stationary cycling) authorised from week 6
- No heavy lifting for 4 weeks
Expected Results
Results timeline
Days 1–3: moderate pain; Week 1: light activities resumed; Weeks 2–3: return to desk work; Week 6: compression vest removed; Month 3: stable final result; Months 6–12: virtually invisible scar
Longevity
Permanent result in the absence of hormonal imbalance and with stable weight
What to expect
- Flat, natural male chest
- Resolution of subareolar sensitivity
- Periareolar scar virtually invisible at 6–12 months
- Exceptional recurrence in the absence of hormonal imbalance
See our results
Discover our patients' transformations
Pricing
Estimated price
Fee upon consultation
This price includes
- Cost depends on the grade of gynecomastia, operative duration, and anaesthesia and clinic stay fees. A detailed, transparent quote is provided at the end of each consultation.
Prices shown are estimates and may vary depending on the complexity of your case. A personalized quote will be provided during your consultation.
Frequently Asked Questions
In pure pseudo-gynecomastia (fatty component only), liposuction may suffice. In mixed gynecomastia, the fibrous glandular tissue cannot be aspirated — it must be excised. Men who underwent liposuction alone and still feel firmness beneath the areola require a corrective surgical excision.
The incision is made along the lower border of the areola, at the junction between the pigmented areolar skin and the surrounding skin. This area heals excellently. At 6–12 months, the scar is generally virtually invisible and blends into the natural areolar border.
Dr Fathi recommends waiting for hormonal stabilisation, generally from the age of 18. Surgery too early risks recurrence if hormones fluctuate subsequently.
If the hormonal or medication cause is controlled and weight is stable, recurrence is very rare after complete glandular excision. Maintaining a constant weight and avoiding androgenic substances (anabolic steroids) is essential for lasting results.
Light activities (walking, stationary cycling) are authorised from week 6. Pectoral bodybuilding and contact sports are not recommended before 3 full months to protect deep-tissue healing.
Questions about gynecomastie-mixte?
Chat directly with our team on WhatsApp for a quick and personalized response.